Read about mesothelioma, including risk factors, symptoms, diagnosis and treatment options.

What is mesothelioma?
Mesothelioma is a rare type of cancer that starts in the mesothelium.
The mesothelium is a thin lining (membrane) that surrounds the space in the chest, abdomen and pelvis (also called the outer lining or parietal lining) and covers and protects most of your internal organs (also called the inner lining or visceral lining).
Between the linings, there is a small amount of fluid that helps your organs to move easily.
Mesothelioma causes the linings to become hard and thicken, causing pain, and making it more difficult for your organs to move.
Risk factors for mesothelioma
Anything that can increase your chances of developing cancer is called a risk factor. Exposure to asbestos is the main risk factor for mesothelioma.
Mesothelioma usually starts at least 15 years after exposure to asbestos. Asbestos is a substance used mainly in insulation, fire proofing and sound proofing. It cannot do any harm until a person is exposed to the tiny fibres that make up the asbestos. This can happen if it is broken or damaged. Asbestos is most likely to be found in buildings built before the mid-1980s.
Types of mesothelioma
- Pleural mesothelioma
Starts in the linings around the lungs (most common, but still rare)
-
Peritoneal mesothelioma
Starts in the linings in and around the abdomen and pelvis (rare) - Pericardial mesothelioma
Starts in the linings around the heart (very rare)
Pleural mesothelioma
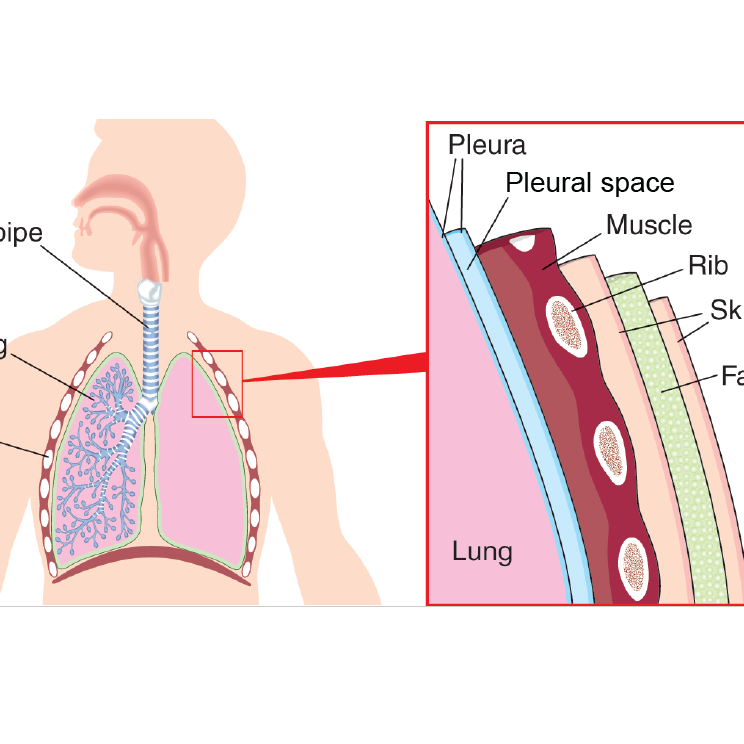
The mesothelium in the part of the chest where the lungs are is called the pleura. Pleural mesothelioma is a cancer that starts in the linings around the lungs.
The gap between the linings is called the pleural space. The gap is filled with a fluid made by the pleura which makes it easier for your lungs to move as you breathe in and out.
Mesothelioma causes the pleura to become hard and thicken. This causes pain and makes it harder for your lungs to move as you breathe.
Sometimes the pleura makes too much fluid. This extra fluid makes it harder for your lungs to move, and you might find it harder to breathe. This is called a pleural effusion.
Symptoms of pleural mesothelioma
The symptoms of pleural mesothelioma may include:
- A cough that doesn’t go away
- Chest pain – usually on one side
- Shortness of breath
- Fatigue (extreme tiredness)
- Weight loss
- Sweating and fevers (increased body temperature)
Pleural mesothelioma and asbestos
Asbestos fibres can be breathed into the smallest parts of your lungs. Some fibres are so small, that they can move through your lungs and out into the lining of the lungs (pleura). Over time, this can develop into pleural mesothelioma.
Peritoneal mesothelioma
The mesothelium in the abdomen and pelvis is called the peritoneum.
The inner (visceral) layer covers the organs such as the bowel and liver. The outer (parietal) layer lines the walls of the abdomen and pelvis (tummy).
Peritoneal mesothelioma is a cancer that starts in the peritoneum and is very rare.
The space between the linings of the peritoneum is filled with fluid that helps protect the organs as you move around.
Mesothelioma causes the lining of the peritoneum to become hard and thicken. Sometimes the amount of fluid in the peritoneum increases. The extra fluid causes swelling in the abdomen and pelvis (tummy) that can be very uncomfortable. This is called ascites.
Side view of the abdomen and pelvis (tummy) showing the peritoneum

Symptoms of peritoneal mesothelioma
The symptoms of peritoneal mesothelioma may include:
- Pain in the abdomen and pelvis (tummy)
- Swelling in the tummy (ascites)
- Feeling sick or being sick
- Weight loss
- Changes in your normal bowel habits such as constipation or diarrhoea
- Night sweats
Diagnosing mesothelioma
If you have noticed any of the symptoms of mesothelioma, you will usually see your GP or whānau doctor first. They will talk to you about your symptoms and ask if you may have been exposed to asbestos in the past.
If your GP is concerned that your symptoms may be signs of mesothelioma, they will recommend further tests.
The results of any tests you have, will help your treatment team to decide what the best treatment options are for you.
Tests may include:
- X-rays
- CT, MRI or PET scans
- Biopsy

Treatment for mesothelioma
Treatment for mesothelioma may include chemotherapy, radiation treatment, immunotherapy, supportive care, and surgery (rare). There is no cure for mesothelioma, so the aim of treatment is to make sure you have good quality of life for as long as possible.
If you have cover through ACC, your cancer doctor can make a request for funding for medications. These requests are assessed on a case-by-case basis.
Chemotherapy
Chemotherapy uses medication to kill cancer cells and slow their growth.
Chemotherapy side effects vary depending on the combination of medications you receive. You can ask your treatment team to provide you with some written information on the side effects that are most likely to affect you.
Common side effects you may experience include:
- Increased risk of infection
- Fatigue
- Forgetfulness and concentration problems (chemo brain)
- Nausea (feeling sick) and vomiting
- Constipation or diarrhoea
- Sore mouth and ulcers
Some side effects of chemotherapy can be life threatening
If you develop any of the following symptoms, you must contact your treatment team or go immediately to your nearest hospital emergency department and tell them you are receiving chemotherapy treatment:
- Fever – a temperature over 38℃
- Chills – shivers or shakes, feeling hot or cold
- Chest pain
- Difficulty breathing
- Vomiting that continues after taking anti-sickness medication
- Diarrhoea
- Gum or nose bleeds or bleeding that does not stop
- Pain or burning when passing urine, or blood in urine
It is important that you do not wait to seek assistance until the next morning or after the weekend.
The availability of immunotherapy for mesothelioma
There have been recent advances in mesothelioma treatment using immunotherapy. These treatments are not yet funded by PHARMAC in New Zealand. You may like to ask your oncologist if there are any unfunded treatments or clinical trials available that may be beneficial for you. Your medical oncologist can give you an estimate of the cost involved if you choose to fund your own treatment.
If you have cover through ACC, your cancer doctor can make a request for unfunded treatments. These requests are assessed on a case-by-case basis.
Radiation treatment
Radiation treatment is the use of x-ray beams to destroy cancer cells or slow their growth. Radiation treatment only affects the part of the body that the beams are aimed at.
For people with pleural mesothelioma, radiation treatment to small areas of the chest can help control pain.
Radiation treatment is not often used to treat peritoneal mesothelioma.
People react in different ways to radiation treatment. These are the common side effects that you may experience:
- Fatigue (tiredness) — can occur during and after treatment
- Red and dry skin in the area being treated
- Nausea (feeling sick) or vomiting
- Loss of appetite
Surgery
For some people with peritoneal mesothelioma, surgery to remove the peritoneum may be considered. This may be combined with chemotherapy placed into the abdomen (tummy) during the surgery. This is called heated intraperitoneal chemotherapy (HIPEC) and is only available in Waikato Hospital, Hamilton (2022).

Supportive care and palliative treatment
Supportive care
Anyone with mesothelioma may need supportive care. It includes the management of physical symptoms, emotional and spiritual support, and guidance to help you plan ahead.
Specialist palliative care
You may need extra support if the symptoms you are experiencing are complex or difficult to manage. Your GP, whānau doctor or cancer treatment team may refer you to a specialist palliative care service.
Palliative care is often provided by primary health care teams as part of supportive care. It is a good idea to ask for palliative care early rather than wait until things become difficult to manage. This can help to reduce stress for you and your whānau.
ACC (Accident Compensation Corporation): Financial assistance
If you have been diagnosed with mesothelioma and you have come in to contact with asbestos in the past, you may be able to apply to ACC for financial assistance.
Any of your doctors can lodge a claim with ACC, who will send you and the doctor a patient information pack. Once this information pack has been completed and returned to ACC, they will usually respond to you within a few days to let you know that they have received your claim.
To receive financial support from ACC, the information provided to ACC must show that you were exposed to asbestos in New Zealand.
The exposure event could either be:
- during paid employment, and the exposure was caused by the type of work you do
- an identifiable environmental or repeated secondary exposure to asbestos. For example, you may have secondary exposure to asbestos from repeatedly washing clothes that have asbestos fibres on them.
If your claim is accepted for cover, they will call you to let you know. When you have cover, ACC may be able to assist with:
- loss of wages
- home help
- transport
- medicines
- equipment
If you are eligible, the earlier your claim is sent to ACC, the faster you will receive financial assistance.
For more information on mesothelioma and where you can find support, you can call 0800 CANCER (226 237) and speak to our experienced information and support staff.

Suggested websites
The suggested websites are not maintained by the Cancer Society of New Zealand. We only suggest sites we believe offer credible and reliable information, but we cannot guarantee that the information on these websites is correct, up to date, or evidence-based medical information.
We know that going through cancer is tough and can raise many questions. You are not alone.
We have health professionals to answer your questions and provide the support you need.
Get in touch
