This information is for people who have cancer that has come back or spread - this is called advanced cancer.
Our 'Living well with advanced cancer' booklet is available now.
Living with advanced cancer can be challenging, both physically and emotionally, for people with cancer and whānau.
If you would like to talk with someone about what support is available in your community, call our Cancer Information Helpline 0800 CANCER (226237) to speak with one of our health professionals.
What is advanced cancer?
Advanced cancer is cancer that has spread from the part of the body where it started (the primary cancer) to another part of the body.
This can happen when cells from the primary cancer break away and move around the body through the blood or lymphatic system. While many of the cells will die, some may settle in a new area and start to grow.
Although the cancer is growing in a different part of the body, it is still named after the primary cancer. For example, if bowel cancer has spread to the liver, it is called advanced bowel cancer.
You may also hear people talk about “liver mets”. “Mets” is short for metastasis, which means the cancer has spread.
For example: “you have bowel cancer with liver mets” means, cells from the primary cancer (in the bowel) have spread to the liver and continued to grow.
Your treatment team may use different words to describe cancer that has spread.
You may hear it called:
- metastatic cancer (mets)
- secondary cancer, or
- stage 4 (IV) cancer.
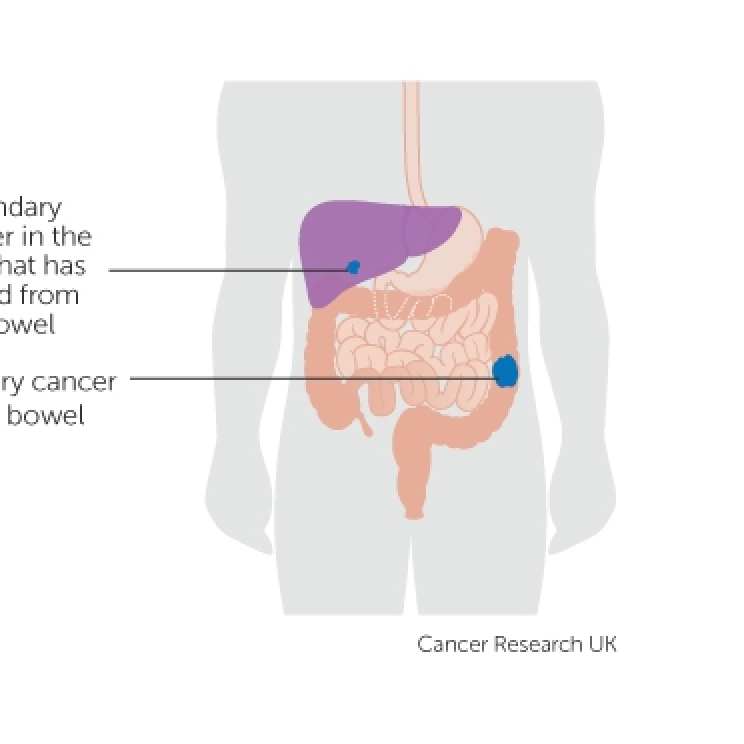
[This image was produced by Cancer Research UK and is used with permission.]
The difference between advanced cancer and terminal cancer
Advanced cancer is a term used to describe cancer that is unlikely to be curable but can be managed with treatment. This is why many people with some types of advanced cancer live well and for a long time.
Terminal cancer is when the cancer is no longer responding to any treatment. Having more treatment or a different treatment is not likely to help. If you have terminal cancer, any medication you are given is to keep you comfortable as you near the end of your life.
Symptoms of advanced cancer
The symptoms of advanced cancer will depend on the part of the body that the cancer has spread to.
For more information about where cancer can spread to, you can read the information in the links below.
Treatment for advanced cancer
Treatment for advanced cancer will depend on the type of cancer you have, where it is in your body and how it will affect you.
The aim is to control the cancer for as long as possible, improve any symptoms, and maintain your quality of life. Sometimes treatment can shrink the size of the cancer or even stop it growing for a while.
Advanced cancer is often managed with more than one type of treatment.
Your treatment may include:
- Chemotherapy
- Hormone treatment
- Immunotherapy
- Radiation treatment
- Specialist palliative care
- Supportive care
- Surgery (in some cases)
- Targeted treatments
- Traditional healing or complementary therapy
Sometimes there will be no benefit in having cancer treatments (such as radiation or chemotherapy), but you will always be offered supportive care.
Supportive care includes the management of physical symptoms, emotional and spiritual support, and guidance to help you plan for the future.
Supportive care will mostly be provided by your primary health care team, Cancer Society support workers, and specialist palliative care services.
If the symptoms you are experiencing are difficult to manage, you and your whānau may be referred to a specialist palliative care service.
Specialist palliative care helps with the physical and emotional needs of people with advanced cancer, and can link you with practical support in your local area. Care can be provided at home or in a hospital, rest home, or hospice by doctors, nurses, social workers, spiritual care workers, and cultural health services.
Advance care planning
An important part of planning ahead is preparing an advance care plan.
Advance care planning helps you, and the people important to you, to talk about the treatment and care you may want towards the end of your life. This will guide your whānau and doctors if you can no longer tell them yourself. Advance care planning is voluntary — no one can force you to do it.
Advanced cancer series
More information on cancer that has spread
Advanced cancer booklets
We know that going through cancer is tough and can raise many questions. You are not alone.
We have health professionals to answer your questions and provide the support you need.
Get in touch
