The treatment offered will depend on the type and stage of the breast cancer, as well as your general health and fitness.
How is breast cancer treated?
Breast cancer can be treated by:
- surgery
- radiation treatment
- chemotherapy
- hormonal therapy
- targeted treatments
Before any treatment begins, make sure that you have discussed and understood your treatment team's advice. You may ask for a second opinion if you want one.
Some treatments for breast cancer can make you unable to get pregnant (infertile). Talk to your treatment team about this before treatment starts.
Some treatments for breast cancer can make you unable to get pregnant, for a short time or permanently.
Talk to your treatment team about this before treatment starts so you have an opportunity to look at what fertility preservation may be available to you. This is the ability to save or protecting eggs, sperm, or reproductive tissue that can be sued in the future to have biological children.
Even with the possibility of infertility, contraception should be used to avoid pregnancy. This is because the treatments used to treat breast cancer could harm a growing baby. Talk to your treatment team about the best contraceptive method for you.
If you are pregnant or think that you may be pregnant, talk to your doctors before starting any cancer treatment. They are there to support you and help you make the best choices for you and your unborn baby.
Tērā pea, ka matapā koe i ētahi o ngā maimoatanga mō te matepukupuku ū, mō te wā poto, mō ake tonu atu rānei. Kōrero ki tō kāhui maimoa e pā ana ki tēnei i mua i te tīmatatanga o ngā maimoa. kia whai wāhi ai koe ki te titiro ki te rāhuitanga ngotongoto tērā pea ka wātea ki a koe.
Ahakoa tērā ka noho matapā koe, me whakamahi tonu i te ārai hapū kia kore ai koe e hapū. Ko te tikanga o tēnei, tērā pea ka whakamamae ngā maimoatanga ka whakamahia mō te maimoa matepukupuku ū, i tētahi pēpi e tipu ana. Kōrero ki tō kāhui maimoa e pā ana ki te huarahi ārai hapū pai ake mōu.
Mehemea kua hapū koe, kei te whakaaro rānei tērā pea kei te hapū koe, kōrero ki ō rata i mua i tō tīmata maimoa matepukupuku. Kai konā rātou ki te āwhina i ā koe ki te whai i ngā whiriwhiringa pai ake mōu me tō pēpi ā-muri.
- Ka taea te maimoa i te matepukupuku o ngā ū mā ngā huarahi maha: te pokanga, te maimoa te iraruke, te haumanu taiaki, me ngā maimoatanga whakahāngai rānei
- Tērā pea, ka matapā koe i ētahi o ngā maimoatanga mō te matepukupuku o ngā ū. Kōrero ki tō kāhui maimoa e pā ana ki te matapā me te ārai hapū i mua i te tīmatatanga o ngā maimoa.
- Whai muri i tētahi tangohanga ū (mastectomy), tērā pea ka āhei koe ki te whai hanganga hou ū.
- He pānga ki te taha tā ngā maimoatanga katoa mō te matepukupuku ū. Kōrero ki tō kāhui maimoa mō te āhua ki te whakahaere i ēnei.
- Matapaki me tō kāhui maimoa me ētahi atu maimoatanga e whakaarotia ana e koe hei whakamahi.
Surgery for breast cancer
There are two kinds of surgery for breast cancer:
Breast-conserving surgery
Breast-conserving surgery where only part of your breast is removed. It is sometimes called a lumpectomy or a wide local excision.
This surgery will leave a scar and may change the appearance of your breast.
Mastectomy
A mastectomy removes the whole breast, as well as some of the skin and the nipple. In some cases, it may be possible to keep the nipple.
After the mastectomy, there will be scarring on your chest. You may be offered breast reconstruction at the same time as your surgery or after any further treatment finishes.
After a mastectomy, it may be possible for you to have more surgery to rebuild your breast, called breast reconstruction.
Some people choose not to have more surgery.
Your treatment team may send you to a plastic or reconstructive surgeon who will discuss breast reconstruction options with you.
There are three main types of reconstruction:
- a breast implant
- a flap reconstruction using your own tissue
- a combination of tissue and an implant
Breast reconstruction may be done at the same time as your mastectomy or a later date.
Breast reconstruction using implants is not recommended for people who are smokers.
Breast reconstruction using flaps of skin and tissue from other areas of your body is not usually recommended for people who have diabetes, are smokers, or are overweight.
You may like to talk to your cancer treatment team about options to help you quit smoking.
After breast cancer surgery
After breast cancer surgery, you may have a small drain in the wound to remove extra fluid into a small container.
Many people go home with this drain still in place. Your treatment team will show you how to care for it, and you may have a community health nurse visit you at home.
The drain will be taken out when it is no longer needed. Follow any instructions given to you by your treatment team and ask them any questions you may have.


The first time you look at your breast or chest after surgery can be overwhelming. Swelling and bruising should settle in a few weeks. In time the scar will flatten and fade.
If lymph nodes were removed during surgery, you might experience shoulder stiffness, nerve pain or numbness in your upper arm, or long-term lymphoedema.
Lymph nodes (also known as glands) are found throughout the body and are part of the lymphatic system.
The lymphatic system contains a series of lymph vessels (tiny channels under the skin) that carry the lymph fluid through the nodes back to the bloodstream.
Lymph nodes contain white blood cells that help fight infection and diseases, such as cancer.
The number of lymph nodes you have is different for each person.
For example, there can be between 15 to 30 nodes in an armpit. Lymph nodes also vary in size from a pinpoint to the size of a baked bean.
Lymph nodes can swell and become tender when you have an infection. If you develop a swollen lymph node, get it checked by your doctor.
Sometimes, cancer cells spread into the lymph nodes from cancer in another part of the body. It is also possible for cancer to start in a lymph node. This type of cancer is called lymphoma.
Chemotherapy for breast cancer
Chemotherapy uses drugs to destroy cancer cells while doing the least possible damage to normal cells.
Chemotherapy may be given for breast cancer:
- If the cancer is hormone receptor-negative
- If the cancer is HER2 positive
- When the risk of cancer returning is high
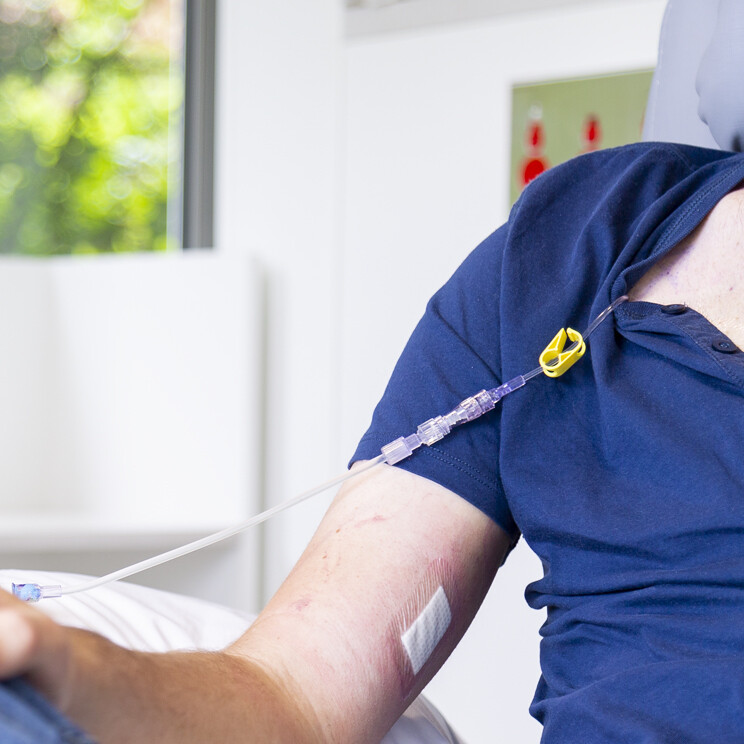
Radiation treatment for breast cancer
Radiation treatment is the use of radiation beams to destroy cancer cells or slow their growth.
Radiation treatment is usually recommended for breast cancer:
- after breast-conserving surgery to reduce the risk of cancer coming back
- before or after a mastectomy, if there is a significant risk of the cancer returning
- if there were cancer cells in the lymph nodes under your armpit
Targeted treatment for HER2 positive breast cancer
Targeted treatments use drugs that work on the damaged genes or proteins of cancer cells to stop the cancer from growing and spreading.
You will be offered targetted treatment if your test results show the breast cancer is HER2 positive.
The most commonly used targeted treatment is trastuzumab (Herceptin).
Pertuzumab (Perjeta) may be offered in some situations but is currently only funded for advanced breast cancer.
Hormone treatments (endocrine therapy)
Some cancer cells respond to the hormones oestrogen and progesterone in your body.
Hormone treatments use these hormones to slow or stop the growth of some cancer.
If your test results show that the breast cancer is hormone receptor-positive cancer, you will be offered hormone treatment.
Palliative care
Palliative care aims to improve your quality of life. It is not just about end of life care.
Palliative care will help:
- you to enjoy the best quality of life you can for as long as possible
- make sure that your physical, practical, emotional and spiritual needs are looked after as well as possible
- manage symptoms of your cancer
- manage side effects of treatment
- help you to feel in control of your situation
- make your time as positive as it can be for you and your family/whānau
Speak with your treatment team about palliative care options for you and your family/whānau.
Life after cancer treatment
After you finish treatment for cancer, give yourself time to adjust to the physical and emotional changes. We are still here to support you after your treatment finishes.
You will need regular check-ups with your treatment team. These may include some blood tests or physical examinations. Speak with your treatment team about the plan for you.

What happens when breast cancer treatment ends?

How to manage the symptoms of cancer and the side effects of treatment.

We are here to help and support you and your whānau through cancer diagnosis, treatment and recovery…

Help with making tough decisions about what treatment you will have.
We know that going through cancer is tough and can raise many questions. You are not alone.
We have health professionals to answer your questions and provide the support you need.
Get in touch
